Tritech supports ‘Bench to Bedside’: Accelerating evidence and value creation
within the NHS to enhance insights, impact, and uptake for patients,
healthcare providers, and industry partners.
rTMS
Repetitive Transcranial Magnetic Stimulation (rTMS) is a type of technology that can be used in treatment for psychiatric conditions. rTMS involves contact between the device and the patient’s head and uses electromagnetic induction to stimulate parts of the brain. This has been shown in clinical studies to be effective. This technology is non-invasive, stimulation of the brain happens through the skull so there is no need for the patient to be under anaesthetic. Following treatment, a patient can drive themselves home.
Cambridge Diabetes Education Programme (CDEP)
Building upon our already established track record of innovation, The TriTech Institute was established by Hywel Dda UHB, mindful of the national and local policy and strategic context, to support the development and evaluation of innovative healthcare technologies, which contribute to improved patient outcomes. Previous work supported by Hywel Dda includes the following.
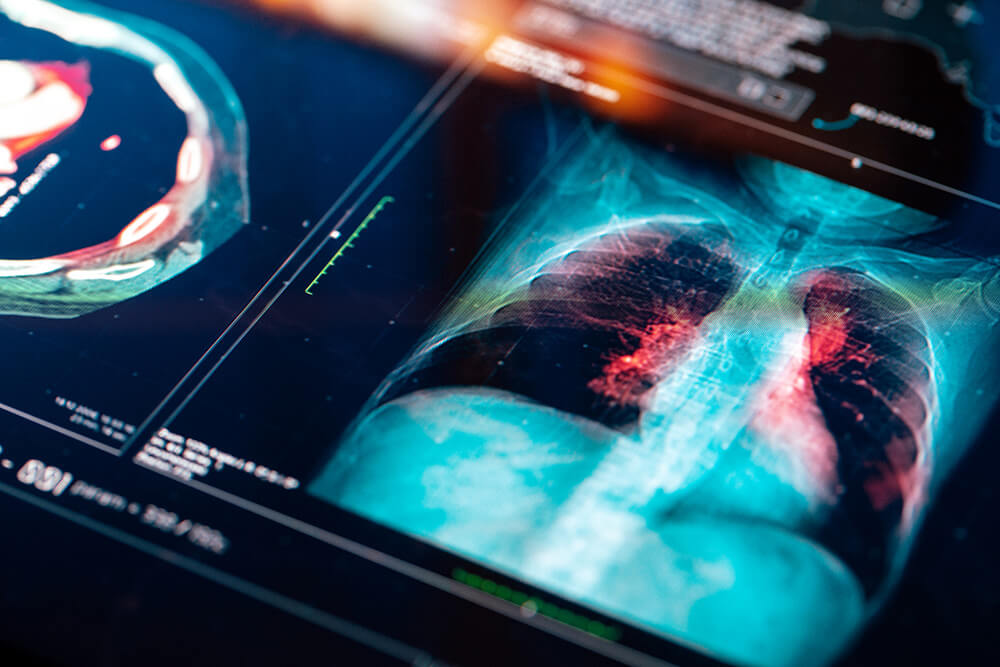
The application of novel technologies to identify new biomarkers for diagnosing and monitoring pulmonary diseases (NovelTech)
The project investigates biomarkers (chemicals in people’s blood, urine, saliva and sputum) that may be detectable before patients develop symptoms or changes are seen on hospital scans and chest X-rays. The project then further explores how biomarkers are affected by changes in a person’s condition or treatment. Information from participants’ medical records are gathered together with samples that undergo i-omics analysis.
Chronic Pain Management E-learning programme: Byw Bywyd Gyda Phoen. Bevan Commission, Swansea University
The project proposes to digitalise our existing, effective 12-module pain management programme, creating a linear programme in a digital format – LMS. Each module will include education around pain, relaxation, goal setting, pacing and exercises as well as additional resources that users could access.

PocketMedic
PocketMedic is a digital platform that allows clinicians in primary, secondary or community care, to send film-based prescriptions to patients to help manage chronic diseases. These can be watched on mobile phones, tablets, or PCs. Over 30 films are now available for type 2, type 1, gestational and pre-diabetes – covering all aspects of diabetes care.

My COPD Pal
To support self-management, in partnership with Bond Digital Health (BDH), Bevan Commission, Swansea University and patient representatives, a digital mobile phone app was developed that allowed patients to take control of their Chronic Obstructive Pulmonary Disease (COPD).

Using video conferencing to extend the benefits of pulmonary rehabilitation to rural communities (VIPAR)
Pulmonary rehabilitation is a programme of exercise and education for patients with Chronic Obstructive Pulmonary Disease (COPD), which traditionally takes place twice a week over a seven-week period. For individuals with a chronic lung condition, Pulmonary Rehabilitation should be an integral part of their care, and the Welsh Government outlined an expectation that all eligible patients are offered such services.
A cloud-based defibrillation system during COVID-19
There are more than 30,000 out-of-hospital cardiac arrests (OHCAs) in the UK each year and the overall survival rate in the UK is just 1 in 10. Every minute without cardiopulmonary resuscitation (CPR) and defibrillation reduces the chance of survival by up to 10%, while performing CPR can more than double the chances of survival in some cases (ventricular fibrillation).

UVC air sterilisation devices as a strategy to reduce airborne transmission risk
During the second wave of the SARS-CoV-2 pandemic, the numbers of patients admitted into hospital rose steadily across the UK from a weekly average of 122 (September 1st 2020) up to 2,037 (17th December) eventually reaching a peak of 4,232 cases per week on 9th January 2021. During this time, the NHS continued to deliver with other non-COVID admissions and elective surgery.